Context & Why Now
Burnout and workforce fragility are no longer background noise; they are now central determinants of health system performance. In 2025, a JAMA Network Open analysis of U.S. health-care workers reported persistently high burnout levels across physicians and nurses, with only modest improvement after the peak COVID years. (JAMA Network) A 2025 umbrella review found that roughly one-third of nurses globally meet criteria for emotional exhaustion, with similar rates for low personal accomplishment. (BioMed Central) Nurse burnout is tightly linked to worse patient safety, satisfaction, and quality outcomes. (JAMA Network)
Canada shows similar strain. The Canadian Medical Association's 2024–2025 National Physician Health Survey reported that nearly half of physicians screened positive for burnout, with administrative burden and inefficient technology among the top drivers. (Canadian Medical Association)
Executive Summary
- •Workforce Crisis: Global shortages, rising burnout, and tightening regulation require treating AI as a workforce instrument, not just a gadget.
- •Evidence-Based Approach: AI can sustainably improve burnout, staffing, and retention only when deployed as an integrated workforce operating system focused on time and fairness.
- •Proven Results: Ambient AI scribes show 0.9-hour reduction in after-hours documentation daily and measurable burnout score improvements. (JAMA Network)
- •Economic Case: For 100 physicians, AI scribes can save ~19,800 hours/year worth ~$3.7M in physician time with payback under 12 months.
- •Regulatory Alignment: EU AI Act (2024), HHS Strategic Plan (2025), and Canadian college guidance provide frameworks for responsible AI workforce deployment.
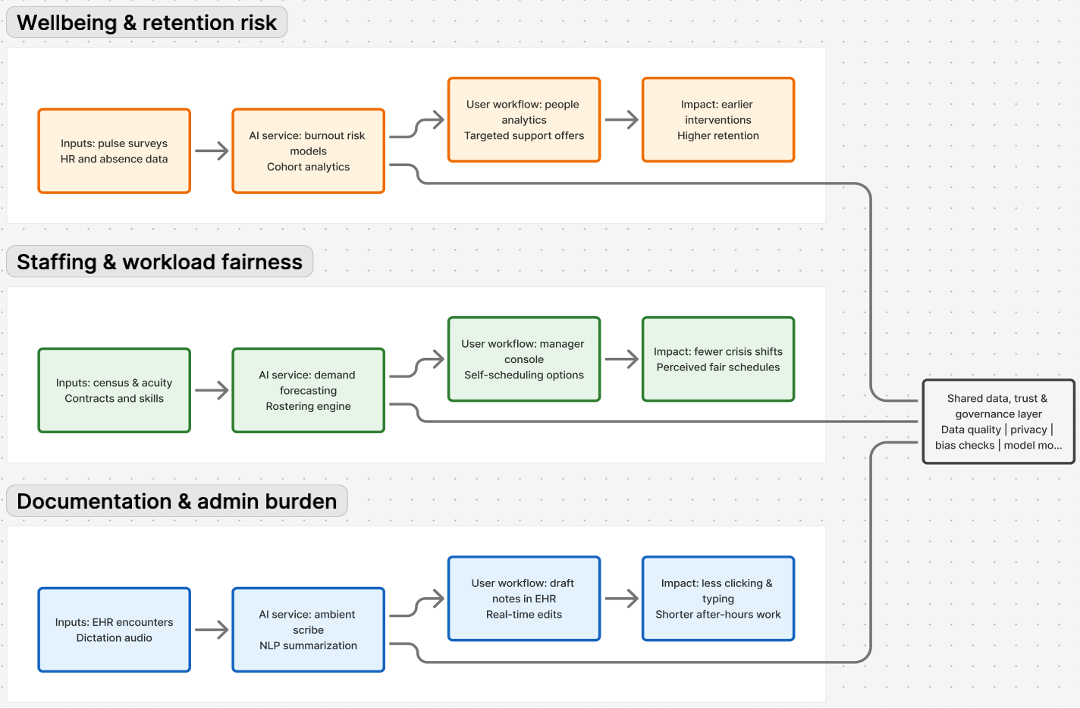
Thesis: AI as a Workforce Operating System, Not a Point Solution
The emerging evidence suggests a simple but non-trivial thesis: AI can sustainably improve burnout, staffing, and retention only when deployed as an integrated workforce operating system whose primary currency is time and fairness, not just productivity.
Ambient Documentation and "Stupid Work" Removal
Randomized and quasi-experimental studies of ambient AI scribes now show measurable reductions in documentation burden and modest improvements in burnout scores. A 2025 multicenter quality-improvement study of ambient AI scribes across six U.S. health systems found a 0.47-point reduction in burnout on a 10-point scale and a 0.9-hour reduction in after-hours documentation per day per clinician after 30 days. (JAMA Network) A separate JAMA Network Open cohort study reported a median 2.4-minute reduction in EHR time per visit and roughly 20 minutes less daily EHR time, including 5 minutes less after hours. (JAMA Network)
Staffing and Rostering Optimization
AI-based nurse scheduling and staffing tools are demonstrating improved perceptions of fairness, transparency, and work–life balance, as well as better matching of staffing to demand. A 2025 BMC Nursing trial found that AI-based scheduling optimized workforce allocation without harming work quality and improved nurse job satisfaction. (BioMed Central) Qualitative work from European hospitals shows that nurses see AI scheduling as potentially enhancing fairness and predictability—if they retain meaningful input into constraints and overrides. (PMC)
Burnout and Attrition Risk Analytics
Beyond logistics, AI is beginning to personalize support. A 2025 three-arm randomized trial of an AI-assisted tailored intervention for nurse burnout showed significant reductions in burnout scores versus control, by delivering individualized wellbeing content and nudges based on self-reported states and usage patterns. (PubMed) Scoping reviews of AI and physician burnout echo this: the most promising tools are those that feed back into workflow redesign rather than merely monitoring stress. (Cureus)
Mini-Case Studies: What Good Looks Like in Practice
Case 1 – The Permanente Medical Group (U.S.): Ambient Scribes at Scale
The Permanente Medical Group (TPMG), serving Kaiser Permanente members in California, rolled out ambient AI scribes at scale beginning in late 2023. By mid-2025, TPMG reported roughly 15,791 hours of documentation time saved over a year after 2.5 million scribe uses, with many physicians self-reporting about one hour per day reclaimed from keyboard work. (American Medical Association)
Case 2 – U.S. Health Systems: Predictive Staffing to Reduce Overtime and Turnover
Several U.S. systems, including Tower Health, Cleveland Clinic, Mayo Clinic, and Mount Sinai, have deployed predictive analytics to better match staffing to patient demand—often using machine-learning models fed by historical census, acuity, and seasonal patterns. These initiatives report reductions in last-minute premium shifts and improved nurse satisfaction with workload balance. (AONL)
Case 3 – Lucerne Cantonal Hospital (Switzerland): AI Scheduling with a European Lens
In 2024, Lucerne Cantonal Hospital (LUKS) in Switzerland introduced an AI-driven scheduling system in partnership with Microsoft Switzerland and Polypoint, positioning itself as one of the first Swiss hospitals to use AI for optimized scheduling. (Source) The system ingests staff contracts, skills, preferences, and expected patient volumes to generate draft rosters that managers and staff can adjust.
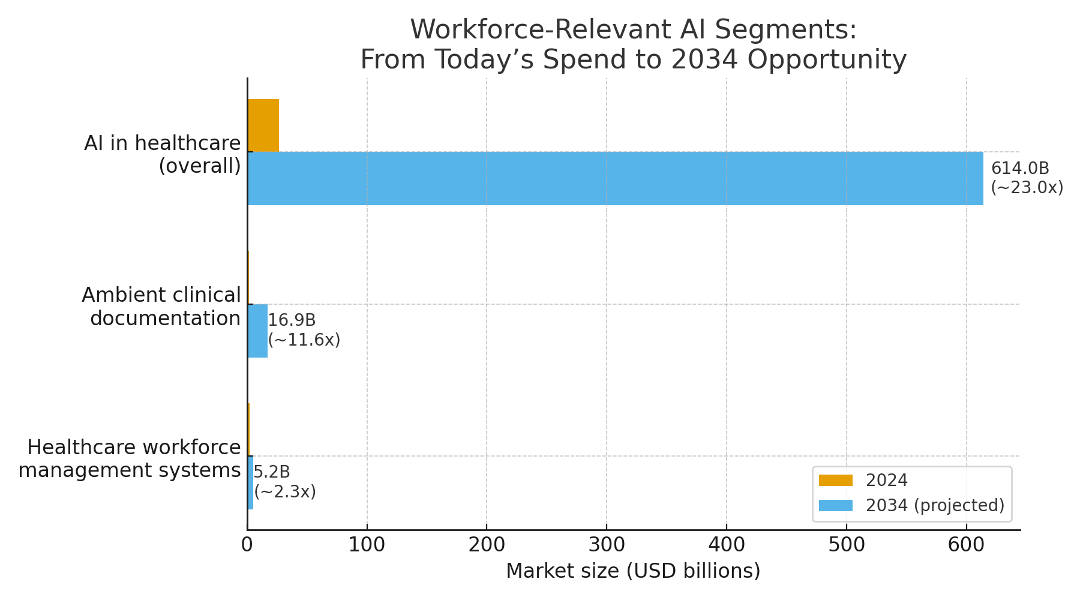
Economics: ROI, Costs, and Time-to-Value
Illustrative ROI for Ambient AI Scribes
- Average U.S. physician compensation: ~$374,000/year ($187/hour)
- Time saved: 0.9 hours/day per clinician (JAMA Network)
- For 100 physicians over 220 days: 19,800 hours/year saved
- Value: $3.7 million in physician time annually
- Typical enterprise AI scribe contracts: low seven-figure range annually
- Payback period: under 12 months when freed hours are redeployed effectively
Risk & Governance: Avoiding New Failure Modes
- Deskilling and over-reliance. A recent randomized trial of AI-assisted colonoscopy reported that clinicians relying heavily on AI missed more lesions when the system was withheld, raising concerns about skill erosion from prolonged automation. (TIME)
- Bias and fairness. AI scheduling systems trained on historical rosters risk codifying existing inequities unless fairness constraints and audit routines are designed in.
- Privacy and cybersecurity. Ambient AI scribes and analytics platforms often process audio, transcripts, and sensitive HR data subject to HIPAA, GDPR, and AI Act obligations.
- Alert fatigue and cognitive load. Poorly tuned AI decision support can increase cognitive burden via excessive alerts or conflicting recommendations.
Implementation Playbook: 90 / 120 / 180 Days
Days 0–90: Baseline, Priorities, and De-risk
- Map current time, burnout, and retention metrics
- Establish AI steering group with clinical, nursing, HR, IT, and legal representation
- Select 1–2 anchor use cases where evidence and pain are strongest
- Conduct vendor due diligence for evidence, privacy, and regulatory compliance
Days 90–120: Pilot with Measurement
- Deploy ambient AI scribes with limited volunteer cohort
- Launch AI-based staffing in single nursing unit with co-design
- Collect pre- and post-measures for time, burnout, and satisfaction
- Target: >20% reduction in after-hours documentation
Days 120–180: Scale and Integrate
- Scale successful AI scribe deployments to additional clinics
- Extend AI staffing tools to additional units with standardized policies
- Integrate data streams into workforce analytics dashboard
- Embed ongoing model monitoring and governance
What to Watch in the Next 12–24 Months
- Higher-quality outcomes data from randomized and controlled studies
- EU AI Act implementation standards and sector-specific guidance
- U.S. Medicare and commercial payer pathways for algorithm-based services
- Pan-Canadian and European guidance on clinician training and liability
- Union and professional-body positions on AI staffing and monitoring
Fact-Check Table
| Claim | Source | Date | Confidence (1–5) |
|---|---|---|---|
| AI scribes reduced burnout scores by ~0.47 on a 10-point scale and cut after-hours documentation by 0.9 h/day | Olson KD et al., JAMA Network Open 2025 | 2025 | 5 |
| AI scribes reduced median EHR time by 2.4 minutes per visit and ~20 minutes per day | Pearlman K et al., JAMA Network Open 2025 | 2025 | 5 |
| TPMG reported 15,791 hours of physician time saved with ambient AI scribes | AMA & TPMG coverage | 2024–2025 | 4 |
| Global nurse emotional-exhaustion prevalence is ~33% | Getie A et al., BMC Nursing 2025 | 2025 | 5 |
| WHO projects ~10–11 million global health-worker shortfall by 2030 | WHO HRH progress report 2024 | 2024 | 5 |
Sources
- Olson KD et al. "Use of Ambient AI Scribes to Reduce Administrative Burden and Professional Burnout." JAMA Network Open. 2025;8(10):e2534976. (JAMA Network)
- Pearlman K et al. "Use of an AI Scribe and Electronic Health Record Efficiency." JAMA Network Open. 2025. (JAMA Network)
- Baek G, Cha C. "AI-Assisted Tailored Intervention for Nurse Burnout: A Three-Group Randomized Controlled Trial." Worldviews on Evidence-Based Nursing. 2025;22(1):e70003. (PubMed)
- Getie A et al. "Global prevalence and contributing factors of nurse burnout: an umbrella review of systematic reviews and meta-analyses." BMC Nursing. 2025. (BioMed Central)
- Li LZ et al. "Nurse Burnout and Patient Safety, Satisfaction, and Quality of Care: A Systematic Review and Meta-analysis." JAMA Network Open. 2024;7(4). (JAMA Network)
- Chen J et al. "Hospital Artificial Intelligence/Machine Learning Adoption in Workforce-Related Areas." Medical Care. 2025;63(3). (Lippincott Journals)
- WHO. "Global Strategy on Human Resources for Health: Workforce 2030 – Progress Report." 2024. (WHO Apps)
- OECD/European Commission. Health at a Glance: Europe 2024. (OECD)
- European Commission. "AI Act enters into force." Press release, 1 Aug 2024. (European Commission)
- HHS. "Strategic Plan for the Use of Artificial Intelligence in Health, Human Services, and Public Health." 2025. (Squarespace)
